Disclaimer: A treatment center will attempt to verify your health insurance benefits and/or necessary authorizations on your behalf. Please note, that this is only a quote of benefits and/or authorization. We cannot guarantee payment or verification eligibility as conveyed by your health insurance provider will be accurate and complete. Payment of benefits is subject to all terms, conditions, limitations, and exclusions of the member’s contract at the time of service. Your health insurance company will only pay for services that it determines to be “reasonable and necessary.” The treatment center will make every effort to have all services preauthorized by your health insurance company. If your health insurance company determines that a particular service is not reasonable and necessary, or that a particular service is not covered under your plan, your insurer will deny payment for that service and it will become your responsibility. We respect your privacy. We request this information to provide you with detailed coverage of benefits. By sharing your phone number, you agree to receive SMS messages via text from us – including details about your benefits. Message and data rates may apply, and frequency varies, text STOP to unsubscribe or HELP for assistance. Sharing this information is not a condition of treatment.
TRICARE Rehab Coverage: Everything You Need To Know
About TRICARE Insurance

TRICARE is the health insurance program for active-duty service members, veterans, military retirees, National Guard and Reserve members, and their families. Managed by the U.S. Department of Defense through the Defense Health Agency, TRICARE provides comprehensive medical, behavioral health, pharmacy, and specialty care coverage both in the United States and overseas.
In addition to routine medical care, TRICARE is widely recognized for its strong support of mental health and substance abuse treatment, including coverage for therapy, psychiatric services, medication-assisted treatment (MAT), detox, inpatient rehab, outpatient programs, and treatment for co-occurring mental health disorders like PTSD, anxiety, depression, and addiction.
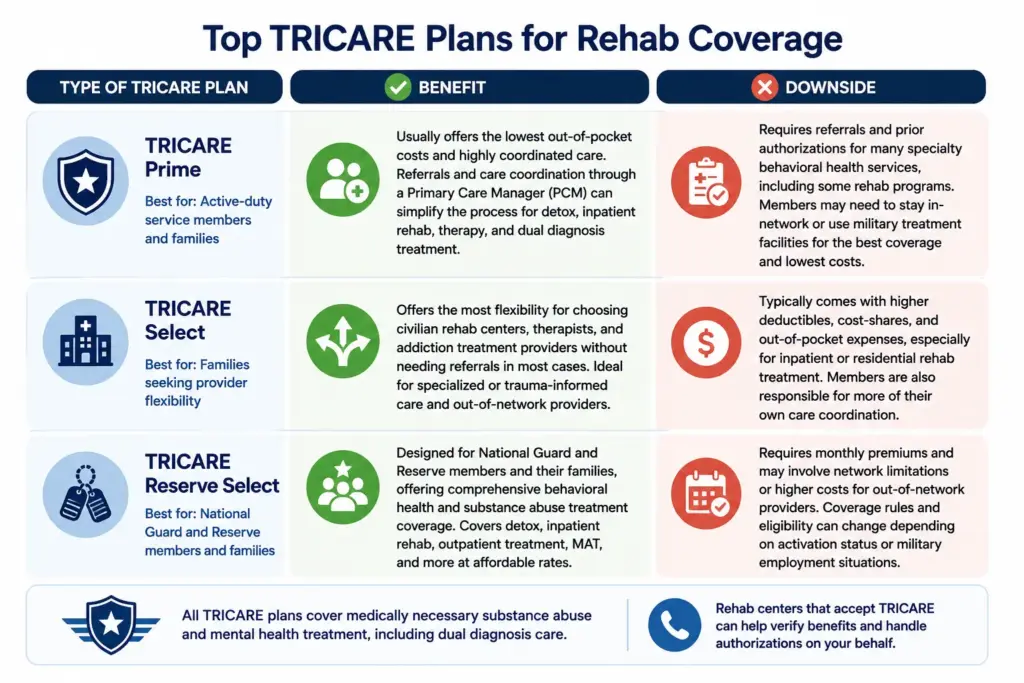
For those searching for TRICARE rehab coverage, the program offers several plan options — including TRICARE Prime, TRICARE Select, TRICARE Reserve Select, and TRICARE For Life — each with different referral rules, provider flexibility, and out-of-pocket costs. Compared to many civilian insurance providers, TRICARE is often viewed as having especially strong behavioral health coverage for military families and veterans, particularly for trauma-informed care and dual diagnosis treatment. TRICARE generally covers medically necessary detox, inpatient rehab, outpatient treatment, Partial Hospitalization Programs (PHPs), Intensive Outpatient Programs (IOPs), and ongoing therapy, though prior authorization is commonly required for residential or inpatient levels of care. Many rehab centers that accept TRICARE can help verify benefits and manage the approval process on behalf of patients to make starting treatment easier and less stressful.
How Does TRICARE Insurance work for substance abuse treatment?
TRICARE works for substance abuse treatment much like a traditional health insurance plan, but it is specifically designed to support military members, veterans, and their families with both addiction recovery and mental health care. When someone seeks treatment, the rehab center or provider typically verifies the patient’s TRICARE benefits, checks whether the facility is TRICARE-authorized, and determines what level of care may be covered. Depending on the plan and medical necessity, TRICARE may help cover detox, inpatient rehab, outpatient treatment, Partial Hospitalization Programs (PHPs), Intensive Outpatient Programs (IOPs), medication-assisted treatment (MAT), therapy, psychiatric care, and treatment for co-occurring disorders like PTSD, anxiety, depression, and addiction. Because trauma and substance abuse are closely linked in military populations, TRICARE is often viewed as one of the stronger insurance options for dual diagnosis and trauma-informed behavioral healthcare.
One important thing to understand is that TRICARE usually requires treatment to be considered “medically necessary,” meaning clinical assessments and documentation may be needed before higher levels of care like residential rehab or inpatient detox are approved. TRICARE Prime plans often require referrals and pre-authorizations for specialty addiction treatment, while TRICARE Select plans generally provide more flexibility in choosing providers without referrals, though out-of-pocket costs may be higher. Many rehab centers that accept TRICARE will handle the insurance verification and authorization process on the patient’s behalf, helping reduce delays during admission. Another unique aspect of TRICARE is its emphasis on continuity of care — meaning coverage may continue through multiple stages of recovery, including detox, rehab, outpatient care, therapy, relapse prevention, and ongoing mental health treatment when clinically appropriate.

Does TRICARE Cover Substance Abuse and Mental Health Disorders?
Yes, TRICARE generally covers both substance abuse treatment and mental health treatment as part of its behavioral health benefits, including care for drug addiction, alcohol addiction, PTSD, depression, anxiety, bipolar disorder, and other mental health conditions. Depending on the plan and medical necessity, TRICARE may help cover detox, inpatient rehab, outpatient treatment, Partial Hospitalization Programs (PHPs), Intensive Outpatient Programs (IOPs), therapy, psychiatric care, medication-assisted treatment (MAT), and virtual mental health services. One area where TRICARE is often viewed especially favorably is its support for dual diagnosis treatment, which helps people receive integrated care for both addiction and mental health disorders at the same time — something that is particularly important for military members, veterans, and families dealing with trauma-related conditions.
Compared to many civilian insurance providers, TRICARE is often recognized for offering strong behavioral health coverage and access to trauma-informed care, especially for active-duty military families and veterans. However, coverage still depends on the specific TRICARE plan, provider network, and whether the treatment is considered medically necessary. TRICARE Prime plans typically require referrals and pre-authorizations for higher levels of care like inpatient rehab, while TRICARE Select plans often provide more flexibility when choosing civilian rehab centers and mental health providers. Because approval requirements can sometimes feel confusing, many rehab centers that accept TRICARE will verify benefits and manage the authorization process on the patient’s behalf before treatment begins.
Does TRICARE Cover Luxury Rehab Treatment?
Yes, TRICARE may cover treatment at a luxury rehab center, but like most insurance providers, it generally only pays for the medically necessary clinical portion of care — not the luxury amenities themselves. This means TRICARE may help cover detox, inpatient rehab, therapy, psychiatric care, medication-assisted treatment (MAT), and dual diagnosis treatment for conditions like PTSD, anxiety, depression, and addiction, even if the treatment takes place at a high-end facility. However, luxury features such as private suites, spa services, gourmet dining, oceanfront accommodations, or concierge-style amenities are usually considered non-essential and are often paid out of pocket. Compared to many civilian insurance providers, TRICARE is often viewed favorably for its strong behavioral health and trauma-informed coverage for military members and families, but it also tends to apply strict medical necessity reviews and prior authorization requirements for inpatient or residential rehab. Many patient experiences online suggest that TRICARE coverage works best when the rehab center is TRICARE-authorized, in-network, and experienced with handling military insurance approvals before admission.
Does TRICARE Cover Residential Rehab Treatment?
Yes, TRICARE does cover residential rehab treatment for substance abuse and co-occurring mental health disorders when the treatment is considered medically necessary and provided through a TRICARE-authorized facility. Depending on the situation, coverage may include medical detox, inpatient residential rehab, therapy, psychiatric care, medication-assisted treatment (MAT), and dual diagnosis treatment for conditions like PTSD, anxiety, depression, or trauma-related disorders alongside addiction recovery. One area where TRICARE stands out compared to many civilian insurance providers is its strong emphasis on trauma-informed behavioral healthcare for military members, veterans, and their families, especially because substance abuse and PTSD often overlap in military populations. However, TRICARE also tends to have stricter clinical review and pre-authorization requirements for residential care, meaning patients usually need assessments and documentation showing that inpatient treatment is medically necessary rather than outpatient care. TRICARE Prime plans typically require referrals and network-based care coordination, while TRICARE Select plans often provide more flexibility when choosing civilian rehab centers. Many rehab facilities that accept TRICARE will handle the insurance verification and authorization process for patients before admission, which can make entering treatment faster and less stressful.
Does TRICARE Cover Outpatient Drug and Alcohol Treatment?
Yes, TRICARE covers outpatient drug and alcohol treatment when it is medically or psychologically necessary and provided by a TRICARE-authorized provider. Covered outpatient options may include individual, family, and group therapy, Intensive Outpatient Programs (IOPs), Partial Hospitalization Programs (PHPs), medication-assisted treatment (MAT), office-based opioid treatment, opioid treatment programs, psychiatric care, and treatment for co-occurring mental health conditions like PTSD, anxiety, depression, or trauma-related disorders.
Outpatient care is often easier to access than residential rehab because it does not require 24/7 supervision, but TRICARE may still require referrals or pre-authorization depending on the plan, beneficiary status, region, and level of care. TRICARE specifically says IOP may be appropriate when someone needs more support than regular outpatient therapy but does not need full-time hospitalization, while PHP is for people who need structured treatment but can still function outside a hospital setting. For best results, patients should confirm the provider is TRICARE-authorized, ask whether Prime or Select rules apply, check if authorization is needed, and have the treatment center verify benefits before starting care.
Additional Information about TRICARE
One thing that makes TRICARE different from many civilian insurance providers is its strong focus on military-related behavioral health and trauma-informed care, especially when handling addiction treatment claims. Because TRICARE serves active-duty military members, veterans, and military families, it is designed with a deeper understanding of conditions that commonly overlap with substance abuse — such as PTSD, combat trauma, anxiety, depression, and chronic stress. This means TRICARE often places a greater emphasis on integrated dual diagnosis treatment, where mental health and addiction are treated together rather than separately.
TRICARE is also known for having more structured clinical review processes than many private insurers. Higher levels of care like detox, residential rehab, and Partial Hospitalization Programs (PHPs) often require detailed medical documentation and prior authorization to prove medical necessity. While this can sometimes make approvals feel stricter, many treatment providers say TRICARE tends to support longer-term continuity of care once treatment is approved, including step-down services like outpatient therapy, medication-assisted treatment (MAT), relapse prevention, and ongoing mental health support. Another major difference is that TRICARE beneficiaries often have access to both civilian rehab centers and military-connected healthcare systems, giving military families more specialized trauma and behavioral health resources than many standard commercial insurance plans.
Personalize your treatment plan
with a benefits specialist. Call us.
Safely Detox at Castillian
Find Alcohol Treatment

Legacy Healing Center Parsippany, NJ

Legacy Healing Center Cincinnati, OH


