Disclaimer: A treatment center will attempt to verify your health insurance benefits and/or necessary authorizations on your behalf. Please note, that this is only a quote of benefits and/or authorization. We cannot guarantee payment or verification eligibility as conveyed by your health insurance provider will be accurate and complete. Payment of benefits is subject to all terms, conditions, limitations, and exclusions of the member’s contract at the time of service. Your health insurance company will only pay for services that it determines to be “reasonable and necessary.” The treatment center will make every effort to have all services preauthorized by your health insurance company. If your health insurance company determines that a particular service is not reasonable and necessary, or that a particular service is not covered under your plan, your insurer will deny payment for that service and it will become your responsibility. We respect your privacy. We request this information to provide you with detailed coverage of benefits. By sharing your phone number, you agree to receive SMS messages via text from us – including details about your benefits. Message and data rates may apply, and frequency varies, text STOP to unsubscribe or HELP for assistance. Sharing this information is not a condition of treatment.
Aetna Rehab Coverage: Everything You Need To Know
About Aetna Insurance

Aetna Insurance, a CVS Health company, offers coverage for addiction treatment to over 36 million people in the US and is considered one of the nation’s leading health insurance providers, offering comprehensive medical and behavioral health plans for individuals dealing with substance abuse.
Known for its broad provider network and integrated healthcare approach, Aetna helps members access mental health services, and substance abuse treatment, including coverage options for drug and alcohol rehab programs.
For those searching for Aetna rehab coverage, Aetna offers a variety of plan types — including HMO, PPO, EPO, POS, and High-Deductible Health Plans (HDHPs) — that may cover detox, inpatient rehab, outpatient treatment, therapy, and medication-assisted treatment (MAT). Coverage levels and out-of-pocket costs vary by plan, but many members can access addiction treatment through Aetna’s extensive behavioral health network, making rehab care more accessible and affordable.
How Does Aetna Insurance work for substance abuse treatment?
Aetna works for substance abuse treatment claims much like other major insurance providers, but many people find its behavioral health system more streamlined because Aetna manages most addiction and mental health services internally rather than outsourcing them to a separate company. In many plans, Aetna covers medically necessary detox, inpatient rehab, outpatient programs, therapy, and medication-assisted treatment (MAT) under the Mental Health Parity and Addiction Equity Act, meaning addiction treatment must be covered similarly to other medical conditions. Members typically need to verify benefits before treatment begins, especially for higher levels of care like detox or residential rehab, where prior authorization is often required.
Compared to some insurance providers that limit behavioral health access through third-party administrators or stricter network restrictions, Aetna often provides broader coordination between medical, pharmacy, and behavioral health services through CVS Health. This can help simplify approvals for rehab, therapy, and medications like Suboxone or Vivitrol. However, coverage still depends on the individual plan, whether the rehab center is in-network, and proof that treatment meets medical necessity guidelines. PPO plans usually offer more flexibility for out-of-network rehab options, while HMO plans tend to require in-network providers to keep costs lower.
Does Aetna Cover Substance Abuse and Mental Health Disorders?
Yes — Aetna generally covers both mental health treatment and substance abuse treatment as part of its behavioral health benefits, and many plans also include care for co-occurring disorders (also called dual diagnosis), where someone is experiencing both a mental health condition and addiction at the same time. Depending on the plan, Aetna may help cover detox, inpatient rehab, outpatient treatment, therapy, psychiatric care, medication management, medication-assisted treatment (MAT), and virtual mental health services. Under federal mental health parity laws, Aetna is required to cover mental health and substance use treatment similarly to physical medical care, which is why many members can access treatment for conditions like depression, anxiety, PTSD, bipolar disorder, and addiction through the same insurance plan.
Compared to some other major insurance providers, Aetna is often viewed favorably for its integrated behavioral health system through CVS Health, broad provider network, and strong support for dual diagnosis care. While insurers like UnitedHealthcare and Cigna also offer solid behavioral health benefits, Aetna stands out for combining medical, pharmacy, and mental health services under one ecosystem, which can make treatment coordination and medication approvals easier for patients. Many plans also include telehealth therapy and online provider tools that simplify finding in-network care. However, coverage still depends on the specific plan, medical necessity requirements, and whether the provider is in-network. PPO plans usually offer the most flexibility for mental health and rehab treatment, while HMO plans tend to have lower costs but stricter network rules.
Does Aetna Cover Luxury Rehab Treatment?
Yes, Aetna may cover luxury rehab treatment, but it typically pays for the medically necessary clinical care, not the luxury extras. That means Aetna rehab coverage may apply to services like medical detox, residential treatment, therapy, psychiatric care, medication-assisted treatment, and co-occurring disorder support when the program meets medical necessity standards. Aetna’s own behavioral health materials note that benefits can include in-person and virtual mental health support, but plans also have exclusions and limitations, so the exact coverage depends on your policy.
Where Aetna can rank well for high-end treatment is with PPO plans, which often provide more flexibility for out-of-network rehab centers than HMO or EPO plans. Compared with some providers that may restrict members to a tighter network or use separate behavioral health administrators, Aetna’s CVS Health connection and national network can make care coordination easier. Still, luxury rehab amenities—private rooms, gourmet meals, spa services, or premium wellness options—are usually paid out of pocket. The best first step is verifying benefits, prior authorization rules, in-network status, out-of-network reimbursement, and whether the facility separates clinical services from private-pay amenities.
Aetna Plans that Cover Rehab
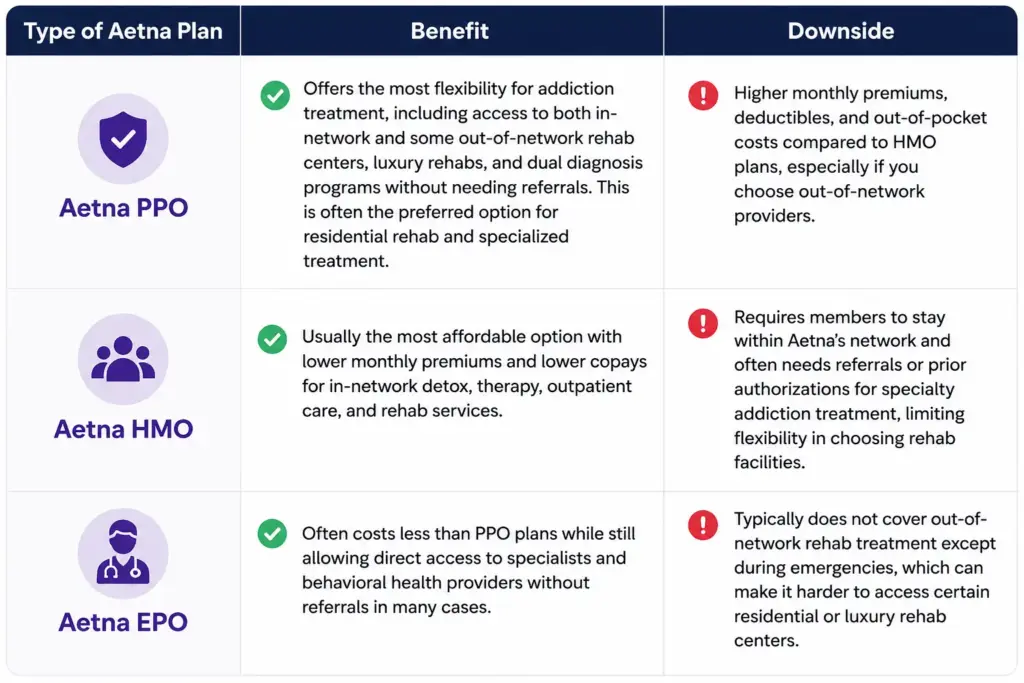
Does Aetna Cover Residential Rehab Treatment?
Yes, Aetna commonly covers residential rehab treatment for drug addiction, alcohol addiction, and co-occurring mental health disorders when treatment is deemed medically necessary. Depending on the specific plan, Aetna rehab coverage may include medical detox, inpatient residential care, therapy, psychiatric treatment, medication-assisted treatment (MAT), and follow-up programs like PHP or IOP care. Aetna typically evaluates residential rehab requests using clinical guidelines such as the ASAM Criteria, meaning approval is often based on withdrawal risk, relapse history, mental health symptoms, unsafe living conditions, or unsuccessful outpatient treatment attempts. PPO plans generally offer the most flexibility for out-of-network rehab centers, while HMO plans may require patients to stay within Aetna’s provider network to maximize coverage and reduce out-of-pocket costs.
Compared to some insurance providers with more restrictive behavioral health systems, Aetna is often recognized for its broad national network and integrated mental health and addiction treatment support through CVS Health. Because many residential rehab programs require prior authorization, patients should verify benefits, deductibles, length-of-stay limits, and dual diagnosis coverage before admission, though many treatment centers can complete this process directly with Aetna on the patient’s behalf.
Does Aetna Cover Outpatient Drug and Alcohol Treatment?
Yes, Aetna often covers outpatient drug and alcohol treatment, including therapy, Intensive Outpatient Programs (IOPs), Partial Hospitalization Programs (PHPs), medication-assisted treatment (MAT), and care for co-occurring mental health disorders like anxiety, depression, or PTSD. The exact amount covered depends on your specific plan and whether the rehab center is in-network, but many people use Aetna insurance to lower the cost of ongoing addiction treatment without needing to stay overnight at a facility. PPO plans usually offer more flexibility for choosing providers, while HMO and EPO plans may require you to stay within Aetna’s network to receive the best coverage. Before starting treatment, it’s always a good idea to verify your benefits and ask the treatment center if prior authorization is needed, since many rehab facilities can handle the insurance approval process for you.
Personalize your treatment plan
with a benefits specialist. Call us.
Safely Detox at Castillian
Find Alcohol Treatment

Legacy Healing Center Parsippany, NJ

Legacy Healing Center Cincinnati, OH


