Disclaimer: A treatment center will attempt to verify your health insurance benefits and/or necessary authorizations on your behalf. Please note, that this is only a quote of benefits and/or authorization. We cannot guarantee payment or verification eligibility as conveyed by your health insurance provider will be accurate and complete. Payment of benefits is subject to all terms, conditions, limitations, and exclusions of the member’s contract at the time of service. Your health insurance company will only pay for services that it determines to be “reasonable and necessary.” The treatment center will make every effort to have all services preauthorized by your health insurance company. If your health insurance company determines that a particular service is not reasonable and necessary, or that a particular service is not covered under your plan, your insurer will deny payment for that service and it will become your responsibility. We respect your privacy. We request this information to provide you with detailed coverage of benefits. By sharing your phone number, you agree to receive SMS messages via text from us – including details about your benefits. Message and data rates may apply, and frequency varies, text STOP to unsubscribe or HELP for assistance. Sharing this information is not a condition of treatment.
Highmark Rehab Coverage: Everything You Need To Know
About Highmark Insurance

Highmark is one of the largest health insurance organizations in the United States and one of the nation’s largest integrated healthcare delivery and financing systems.
As an independent licensee of the Blue Cross Blue Shield Association, Highmark serves millions of members through employer-sponsored plans, individual and family coverage, Medicare, Medicaid, dental, vision, and behavioral health benefits across Pennsylvania, Delaware, West Virginia, and parts of New York. Highmark is part of Highmark Health, a nonprofit health and wellness organization that combines insurance services with provider systems like Allegheny Health Network (AHN), creating a more connected healthcare experience between insurance coverage, hospitals, physicians, behavioral healthcare, and community support services. Highmark publicly describes itself as one of the nation’s largest “blended health organizations,” integrating insurance, hospitals, physicians, technology, and care management into one system focused on improving health outcomes and lowering healthcare costs.
For those researching Highmark rehab coverage, many Highmark plans include behavioral health benefits such as therapy, psychiatry, medication-assisted treatment (MAT), detox, inpatient rehab, outpatient addiction treatment, virtual behavioral healthcare, and treatment for co-occurring mental health disorders like anxiety, depression, PTSD, trauma, and substance use disorders. One thing that makes Highmark especially unique compared to many insurers is its strong emphasis on integrated behavioral healthcare, combining mental health, addiction treatment, primary care, crisis support, digital tools, and care navigation into a coordinated system through Highmark Health and Allegheny Health Network. Highmark and AHN have invested heavily in behavioral health expansion, community mental health programs, virtual care access, and evidence-based psychiatric services designed to improve access to treatment before mental health or addiction conditions reach crisis levels. Many providers and patients online describe Highmark as offering strong provider access and behavioral health resources overall, though prior authorization and medical necessity reviews are commonly required for higher levels of care like detox, inpatient rehab, residential treatment, PHP, and IOP programs.
How Does Highmark Insurance work for substance abuse treatment?
Highmark works for substance abuse treatment by providing coverage for a full continuum of addiction and behavioral health services through its Blue Cross Blue Shield networks and integrated behavioral healthcare programs. Depending on the specific Highmark plan, coverage may include medical detox, inpatient rehab, residential treatment, Partial Hospitalization Programs (PHPs), Intensive Outpatient Programs (IOPs), outpatient therapy, medication-assisted treatment (MAT), psychiatric care, telehealth behavioral health services, and support for co-occurring mental health conditions like anxiety, depression, PTSD, trauma, or bipolar disorder alongside addiction recovery. Highmark’s own substance use disorder resources emphasize that treatment is not one-size-fits-all and that care may involve a combination of psychotherapy, medication, support groups, rehabilitation programs, and ongoing mental health treatment depending on the severity of the condition. Highmark also places a strong emphasis on early assessment, integrated diagnosis, and reevaluating treatment plans when addiction may be connected to underlying psychiatric or trauma-related conditions.
What makes Highmark different from many insurance providers is its integration with Highmark Health and Allegheny Health Network (AHN), which allows the company to coordinate insurance benefits, hospitals, behavioral healthcare, physicians, crisis support, and digital health resources under one broader healthcare system. Many providers and patients online describe Highmark as having strong behavioral health provider access and relatively comprehensive addiction treatment coverage, especially in Pennsylvania and surrounding Highmark markets, though prior authorization and medical necessity reviews are commonly required for detox, inpatient rehab, residential treatment, PHP, and IOP programs. Providers frequently note that approvals tend to move more smoothly when facilities submit detailed ASAM-based clinical documentation showing withdrawal risk, relapse history, failed outpatient treatment attempts, and co-occurring psychiatric symptoms. Highmark also increasingly supports virtual behavioral healthcare and telehealth recovery services, which many patients online say makes it easier to continue therapy, MAT, psychiatry, and relapse prevention after leaving inpatient treatment. One important thing to know is that Highmark coverage can vary significantly by plan type, PPO plans generally provide broader rehab flexibility, while HMO and employer-specific plans may have stricter network and authorization rules, so experienced treatment centers often verify benefits and obtain precertification before admission to reduce delays and unexpected costs.
Does Highmark Cover Substance Abuse and Mental Health Disorders?

Yes, Highmark generally covers substance abuse treatment, mental health treatment, and dual diagnosis care, and the company has become increasingly focused on integrated behavioral healthcare compared to many traditional insurance providers. Depending on the specific Highmark plan, members may have coverage for medical detox, inpatient rehab, residential treatment, Partial Hospitalization Programs (PHPs), Intensive Outpatient Programs (IOPs), outpatient therapy, medication-assisted treatment (MAT), psychiatric care, telehealth behavioral health services, and recovery support programs. Highmark’s own behavioral health resources specifically recognize substance use disorders as medical conditions requiring individualized treatment plans that may combine therapy, medication, rehabilitation programs, and long-term support. Unlike some insurers that separate addiction treatment from mental health services, Highmark increasingly promotes coordinated behavioral healthcare through Highmark Health and Allegheny Health Network (AHN), which allows members in many markets to access more connected mental health, addiction, primary care, and crisis support services under one healthcare system.
For mental health disorders, Highmark commonly covers treatment for anxiety, depression, PTSD, bipolar disorder, OCD, trauma-related disorders, eating disorders, schizophrenia, and other psychiatric conditions through therapy, psychiatry, medication management, inpatient psychiatric care, and virtual mental health programs. Highmark has also invested heavily in digital mental health services, including virtual therapy access and behavioral health navigation programs designed to reduce wait times and improve access to care. Some Highmark plans now offer mental health navigation tools and digital support platforms powered through partnerships like Spring Health, which many members online describe as one of Highmark’s stronger behavioral health advantages compared to more traditional insurance models. Patients and providers frequently describe Highmark as having broad provider access and relatively comprehensive behavioral health benefits overall, especially within Highmark’s core service regions, though prior authorization and medical necessity reviews are still commonly required for higher levels of care like detox, inpatient rehab, residential treatment, PHP, and IOP services.
For people with dual diagnosis conditions, where addiction and mental health disorders occur at the same time, Highmark often covers integrated treatment programs specifically designed to address both conditions together. This can include treatment for addiction alongside PTSD, depression, anxiety, bipolar disorder, trauma, or other psychiatric conditions within the same rehab or outpatient program. Many treatment providers online note that Highmark tends to approve dual diagnosis treatment more successfully when facilities submit strong ASAM-based clinical documentation showing both substance use severity and psychiatric symptoms requiring integrated care. Highmark’s own behavioral health materials emphasize coordinated care and individualized treatment planning rather than treating addiction and mental illness separately, which aligns with current best practices for co-occurring disorders. Compared to many smaller insurers or narrow-network HMOs, Highmark’s Blue Cross Blue Shield network structure often provides broader access to behavioral health providers and multi-level treatment options across inpatient, outpatient, and virtual settings. However, many providers still recommend verifying benefits and precertification requirements before treatment begins because employer-sponsored Highmark plans, Medicare plans, and Medicaid-managed Highmark products can all have different behavioral health rules and network structures.
Does Highmark Cover Luxury Rehab Treatment?
Yes, Highmark may cover treatment at a luxury rehab center, but coverage is usually based on whether the addiction or mental health treatment itself is medically necessary, not whether the facility offers upscale amenities. Depending on the specific Highmark plan, coverage may include medical detox, inpatient rehab, residential treatment, psychiatric care, medication-assisted treatment (MAT), PHP, IOP, and dual diagnosis treatment for co-occurring mental health disorders like anxiety, depression, PTSD, or trauma, even when treatment takes place at a high-end facility. However, private suites, spa treatments, gourmet dining, concierge transportation, executive accommodations, and other luxury features are typically considered non-medical expenses and are generally not covered. Highmark’s authorization and behavioral health guidelines show that residential rehab, withdrawal management, psychiatric residential care, and many higher levels of behavioral health treatment commonly require prior authorization and medical necessity review before coverage is approved.
Many providers and patients online describe Highmark as having stronger behavioral health provider access than many regional insurers because of its Blue Cross Blue Shield network structure and integrated behavioral healthcare system through Highmark Health and Allegheny Health Network. At the same time, people frequently mention that residential rehab approvals can feel highly structured, with ongoing utilization reviews and step-down recommendations after stabilization. Providers who regularly work with Highmark often note that luxury rehab approvals are most successful when facilities submit detailed ASAM-based documentation showing withdrawal risks, failed outpatient attempts, relapse history, psychiatric symptoms, and the need for 24/7 care. One important tip many admissions teams recommend is asking the facility to separate the clinical treatment costs from luxury amenity costs before admission, because Highmark may reimburse medically necessary treatment while leaving resort-style upgrades as private-pay expenses. Patients online also commonly recommend verifying whether the facility is fully in-network before admission, since out-of-network residential rehab can significantly increase out-of-pocket costs even when treatment itself is approved.
Does Highmark Cover Residential Rehab Treatment?
Yes, Highmark commonly covers residential rehab treatment for substance use disorders and co-occurring mental health conditions when the treatment is medically necessary and approved through its behavioral health review process. Depending on the specific Highmark plan, coverage may include medical detox, residential rehab, psychiatric care, medication-assisted treatment (MAT), therapy, PHP, IOP, and integrated dual diagnosis treatment for conditions like anxiety, depression, PTSD, trauma, or bipolar disorder alongside addiction recovery. Highmark’s behavioral health authorization guidelines specifically reference coverage pathways for withdrawal management, psychiatric residential treatment, and residential substance use rehab, with medical necessity reviews commonly based on ASAM Criteria and clinical documentation. Many providers and patients online describe Highmark as having relatively strong behavioral health access compared to smaller regional insurers because of its Blue Cross Blue Shield network structure and integration with Highmark Health and Allegheny Health Network, though residential treatment approvals are often highly structured and reviewed in stages. Providers frequently note that approvals tend to move more smoothly when facilities clearly document relapse history, withdrawal risk, failed outpatient attempts, psychiatric symptoms, and the need for 24/7 supervised care. One important thing many patients mention online is that verifying whether a facility is fully in-network before admission can significantly reduce costs, since out-of-network residential rehab may still lead to large deductibles or balance billing even when treatment itself is approved.
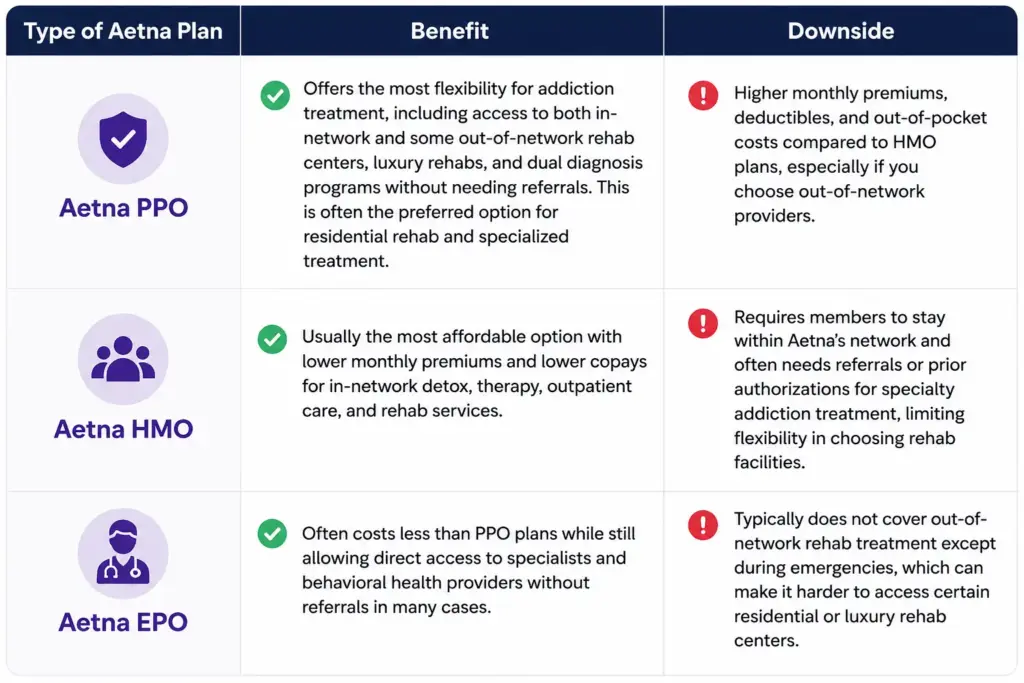
Does Highmark Cover Outpatient Drug and Alcohol Treatment?
Yes, Highmark commonly covers outpatient drug and alcohol treatment, and many Highmark plans place a strong emphasis on outpatient and step-down behavioral healthcare as part of long-term recovery support. Depending on the specific plan, coverage may include standard outpatient therapy, psychiatry, medication management, medication-assisted treatment (MAT), Intensive Outpatient Programs (IOPs), Partial Hospitalization Programs (PHPs), relapse prevention, virtual therapy, family counseling, and treatment for co-occurring mental health disorders like anxiety, depression, PTSD, trauma, or bipolar disorder alongside addiction recovery. Highmark’s behavioral health resources specifically support virtual and telehealth behavioral health programs for conditions including alcohol use disorder, depression, anxiety, OCD, PTSD, and panic disorders, which many members online describe as one of Highmark’s stronger behavioral health advantages compared to more traditional regional insurers.
Many providers and patients online note that outpatient care is often easier to obtain approval for than residential rehab because it allows members to continue working, attending school, or caring for family while receiving treatment. However, higher-intensity outpatient programs like PHP and IOP may still require prior authorization and ongoing medical necessity reviews depending on the plan. Providers who regularly work with Highmark frequently mention that approvals tend to move more smoothly when facilities document relapse risk, failed lower levels of care, psychiatric symptoms, or the need for structured outpatient treatment using ASAM Criteria. Highmark PPO plans generally provide broader access to outpatient behavioral health providers and some out-of-network flexibility, while HMO and employer-sponsored plans may require members to stay within network providers for the best coverage. One important thing many patients mention online is that Highmark’s integration with Highmark Health and Allegheny Health Network often makes transitions between detox, outpatient therapy, MAT, psychiatry, and virtual care more coordinated than with many standalone insurance companies, especially within Highmark’s core service regions.
Additional Information about Highmark
One of the most important things to know about Highmark is that it is not just an insurance company, it is part of an integrated healthcare system through Highmark Health and Allegheny Health Network (AHN), which gives it a very different approach to detox, rehab, and behavioral healthcare compared to many traditional insurers. Instead of only approving claims and managing networks, Highmark is directly connected to hospitals, physicians, psychiatric programs, telehealth systems, crisis services, outpatient programs, and care coordination teams. This integrated structure allows many Highmark members, especially within Pennsylvania and surrounding regions, to move more smoothly between detox, inpatient rehab, outpatient therapy, psychiatry, medication-assisted treatment (MAT), and virtual behavioral health services inside one connected system. Highmark and AHN publicly emphasize “whole-person” and proactive behavioral healthcare, with treatment models that integrate mental health, addiction recovery, trauma treatment, primary care, and telehealth support rather than treating addiction as a short-term isolated condition.
Another especially valuable thing to know is how heavily Highmark has invested in virtual behavioral health and telehealth recovery support, which many providers say is one of Highmark’s biggest advantages for long-term addiction recovery. Highmark’s behavioral health resources include virtual therapy, psychiatric evaluations, digital mental health tools, opioid treatment support, virtual behavioral health vendors, and telehealth MAT programs for opioid use disorder. Highmark-affiliated behavioral health leaders have publicly stated that approximately 80% of behavioral health appointments within AHN continue to be telehealth-based, with 96% patient satisfaction ratings for video services after the pandemic accelerated behavioral health telemedicine adoption. Highmark has also expanded partnerships for virtual opioid treatment and MAT access, including telehealth-based opioid recovery programs for Medicaid and Medicare populations. Many patients online say this continued virtual support after detox or rehab is especially helpful because relapse risk is often highest during the transition back into everyday life, and Highmark’s telehealth ecosystem makes it easier to stay connected to therapy, psychiatry, MAT, and recovery support without gaps in care.
Personalize your treatment plan
with a benefits specialist. Call us.
Safely Detox at Castillian
Find Alcohol Treatment

Legacy Healing Center Parsippany, NJ

Legacy Healing Center Cincinnati, OH


