Disclaimer: A treatment center will attempt to verify your health insurance benefits and/or necessary authorizations on your behalf. Please note, that this is only a quote of benefits and/or authorization. We cannot guarantee payment or verification eligibility as conveyed by your health insurance provider will be accurate and complete. Payment of benefits is subject to all terms, conditions, limitations, and exclusions of the member’s contract at the time of service. Your health insurance company will only pay for services that it determines to be “reasonable and necessary.” The treatment center will make every effort to have all services preauthorized by your health insurance company. If your health insurance company determines that a particular service is not reasonable and necessary, or that a particular service is not covered under your plan, your insurer will deny payment for that service and it will become your responsibility. We respect your privacy. We request this information to provide you with detailed coverage of benefits. By sharing your phone number, you agree to receive SMS messages via text from us – including details about your benefits. Message and data rates may apply, and frequency varies, text STOP to unsubscribe or HELP for assistance. Sharing this information is not a condition of treatment.
Meritain Rehab Coverage: Everything You Need To Know
About Meritain Insurance

Meritain Health is one of the largest third-party administrators (TPAs) in the United States, specializing in self-funded employee health benefits for employers, unions, school systems, and public organizations.
Founded in 1983 and now part of the Aetna and CVS Health family, Meritain combines the flexibility of customized employer-sponsored health plans with access to large national healthcare networks and behavioral health resources. Unlike traditional insurance companies that fully insure employer plans, Meritain primarily administers self-funded health plans, meaning employers often have more control over how benefits are designed and managed. Through its connection to Aetna and CVS Health, many Meritain members gain access to nationwide provider networks, pharmacy services, virtual healthcare tools, and behavioral health support programs.
For those researching Meritain rehab coverage or behavioral health benefits, many Meritain plans include coverage for substance abuse treatment, mental health treatment, therapy, psychiatry, medication-assisted treatment (MAT), detox, inpatient rehab, outpatient programs, and care for co-occurring mental health disorders like anxiety, depression, PTSD, or addiction. One thing that makes Meritain unique compared to many traditional insurance companies is that coverage can be highly customized because plans are employer-designed rather than one standardized national policy. Many Meritain plans use the Aetna Choice® POS II network, which includes access to over 1.6 million healthcare providers and more than 350,000 behavioral health providers nationwide. Meritain also places a growing emphasis on virtual behavioral healthcare, care coordination, and member navigation tools designed to simplify access to mental health and addiction treatment. Many providers and members online describe Meritain as offering strong network flexibility through Aetna-backed provider access, though prior authorization and employer-specific plan rules can still play a major role in behavioral health coverage decisions.
How Does Meritain Insurance work for substance abuse treatment?
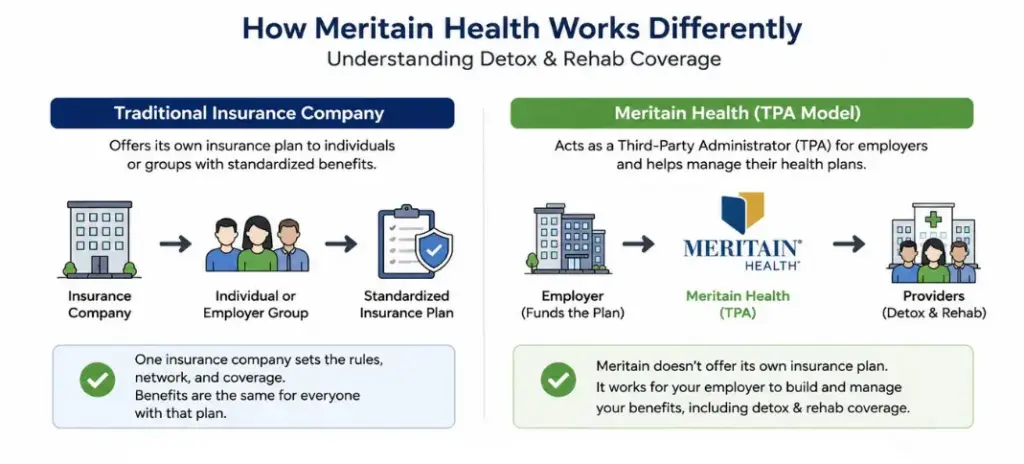
Meritain Health works for substance abuse treatment differently than many traditional insurance companies because it primarily acts as a third-party administrator (TPA) for employer-funded health plans rather than offering one standardized national insurance policy. In most cases, Meritain members access addiction and mental health treatment through the large Aetna Choice® POS II network, giving members access to nationwide detox centers, residential rehab facilities, outpatient programs, therapists, psychiatrists, medication-assisted treatment (MAT), and dual diagnosis providers. Depending on the employer’s plan design, Meritain may help cover medical detox, inpatient rehab, Partial Hospitalization Programs (PHPs), Intensive Outpatient Programs (IOPs), outpatient therapy, psychiatric care, virtual behavioral health services, and treatment for co-occurring mental health conditions like anxiety, depression, PTSD, or trauma alongside addiction recovery. Because Meritain plans are employer-customized, coverage details, deductibles, network rules, and authorization requirements can vary more than with fully insured national carriers.
What makes Meritain unique for addiction treatment is its combination of self-funded employer flexibility with Aetna-backed provider access and behavioral health infrastructure. Many treatment providers online describe Meritain as offering strong nationwide rehab access because members can often use the same large provider network associated with Aetna and CVS Health. However, because employers help design the plan structure, two people with Meritain insurance may have very different rehab benefits depending on their employer’s specific contract. Many rehab providers report that prior authorization, medical necessity reviews, and verification of employer-specific behavioral health benefits are especially important with Meritain claims, particularly for detox, residential rehab, PHP, and IOP levels of care. Providers also note that approvals often move more smoothly when facilities submit detailed ASAM-based clinical documentation explaining withdrawal risks, relapse history, failed outpatient attempts, and co-occurring mental health conditions. Many patients and providers online say the most important step before treatment is having the rehab center perform a full benefit verification because Meritain plans can vary widely in out-of-pocket costs, out-of-network coverage, and behavioral health carve-outs.
Does Meritain Cover Substance Abuse and Mental Health Disorders?
Yes, Meritain Health generally covers substance abuse treatment, mental health treatment, and dual diagnosis care, but coverage works somewhat differently than with many traditional insurance companies because Meritain primarily administers self-funded employer health plans rather than offering one standardized national policy. Most Meritain members access care through the large Aetna Choice® POS II network, which includes more than 350,000 behavioral health providers nationwide and gives members access to detox centers, residential rehab programs, therapists, psychiatrists, medication-assisted treatment (MAT), virtual behavioral healthcare, and outpatient addiction treatment programs. Depending on the employer’s plan design, Meritain may help cover medical detox, inpatient rehab, outpatient therapy, Partial Hospitalization Programs (PHPs), Intensive Outpatient Programs (IOPs), psychiatric treatment, and recovery support services for conditions like alcohol addiction, opioid addiction, stimulant addiction, prescription drug misuse, and other substance use disorders.
For mental health disorders, many Meritain plans provide coverage for therapy, psychiatry, inpatient psychiatric treatment, medication management, trauma treatment, virtual counseling, and behavioral health support for conditions like anxiety, depression, PTSD, bipolar disorder, eating disorders, OCD, and other mental health conditions. Because Meritain is connected to Aetna and CVS Health infrastructure, many plans also support integrated behavioral healthcare models, telehealth behavioral health services, and coordinated care navigation. However, one very important thing to understand is that Meritain coverage can vary significantly from one employer to another because employers help design the benefits structure. This means two people with Meritain insurance may have very different mental health copays, deductibles, provider networks, authorization requirements, or out-of-network behavioral health benefits even though both have “Meritain” cards. Many providers online describe Meritain as having strong network access through Aetna-backed provider systems, but they also stress the importance of verifying benefits before treatment because behavioral health carve-outs and precertification requirements are common.
For people with dual diagnosis conditions, where addiction and mental health disorders occur at the same time, Meritain plans often cover integrated treatment programs designed to address both conditions together rather than separately. This can include treatment for addiction combined with PTSD, trauma, depression, anxiety, bipolar disorder, or other psychiatric conditions within the same rehab or outpatient program. Many rehab providers note that Meritain approvals for higher levels of care like detox, residential rehab, PHP, or IOP tend to go more smoothly when facilities submit detailed ASAM-based clinical documentation explaining relapse risk, psychiatric symptoms, withdrawal concerns, failed outpatient attempts, and the need for structured integrated treatment. Some Meritain/Aetna plan documents specifically list coverage for inpatient behavioral health treatment, psychiatric hospitals, residential treatment facilities, and behavioral health providers, including medically necessary room and board during approved inpatient behavioral health stays. Many providers and patients online also say one of the biggest advantages of Meritain is access to the broad Aetna behavioral health network, while one of the biggest frustrations can be variability in employer-specific plan rules and authorization processes.
Does Meritain Cover Luxury Rehab Treatment?
Yes, Meritain Health may cover treatment at a luxury rehab center when the addiction or mental health treatment is considered medically necessary and included under the member’s employer-sponsored plan, but coverage typically applies only to the clinical services, not the luxury amenities themselves. Because Meritain is an Aetna-owned third-party administrator (TPA), many members use the large Aetna Choice® POS II network to access detox, residential rehab, psychiatric care, medication-assisted treatment (MAT), PHP, IOP, therapy, and dual diagnosis treatment at facilities nationwide, including some upscale programs. However, private suites, concierge services, spa treatments, gourmet dining, and other resort-style amenities are usually considered non-medical expenses and are not covered. One important thing to know is that Meritain coverage can vary significantly depending on the employer’s specific plan design, meaning two people with Meritain insurance may have very different out-of-network benefits, deductibles, and luxury rehab coverage even though both use Meritain. Many rehab providers also note that prior authorization and ASAM-based medical necessity reviews are especially important for residential and luxury rehab claims, so having the treatment center verify benefits and separate clinical costs from luxury amenity costs before admission can help avoid unexpected expenses.
Does Meritain Cover Residential Rehab Treatment?
Yes, Meritain Health may cover residential rehab treatment for substance use and co-occurring mental health disorders when the care is medically necessary and included in the member’s employer-sponsored plan. Because Meritain is an Aetna-owned third-party administrator, many members use the Aetna Choice® POS II network, which Meritain says is chosen by over 90% of its plan sponsors and includes access to 1.6 million providers nationwide, including more than 350,000 behavioral health providers. Coverage may include residential treatment, medical detox, therapy, psychiatric care, medication-assisted treatment (MAT), and dual diagnosis support, but benefits vary more than with many standard insurers because each employer can customize the plan.
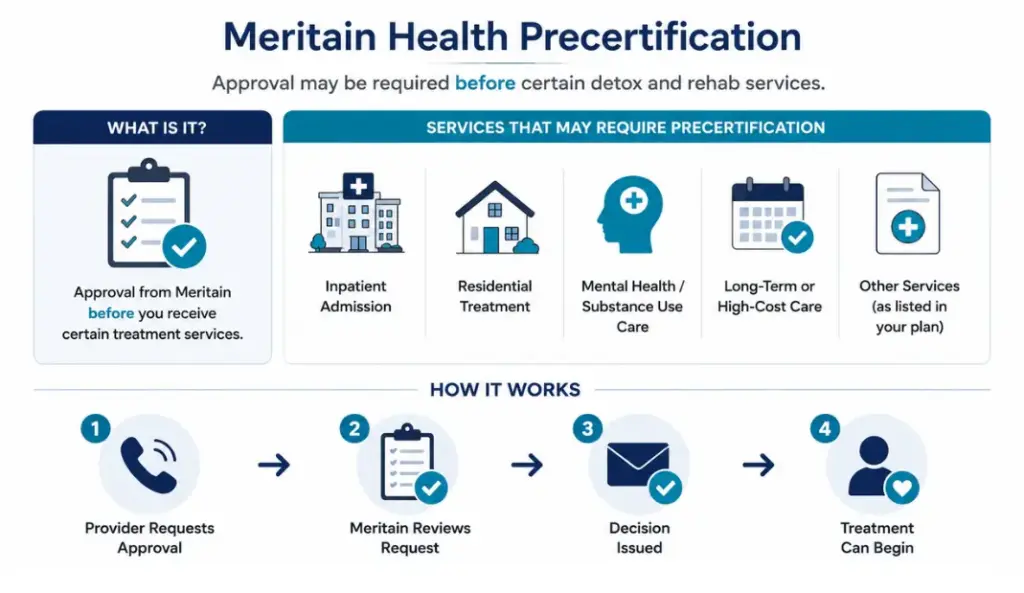
The biggest thing to know is that residential rehab usually requires precertification or prior authorization. Meritain’s own precertification resources list inpatient admissions, mental health/substance use disorder care, and residential treatment facilities as services that may require review before treatment is approved. Online provider feedback generally describes Meritain as strong for network access but highly plan-specific, meaning approvals and costs can differ widely from one employer group to another. Before admission, ask the rehab center to verify your Meritain benefits, confirm Aetna network status, check out-of-network coverage, estimate deductibles and copays, and submit ASAM-based clinical documentation showing why 24/7 residential care is needed.
Does Meritain Cover Outpatient Drug and Alcohol Treatment?
Yes, Meritain Health commonly covers outpatient rehab treatment for drug and alcohol addiction, but the exact benefits depend on the employer-funded plan. Coverage may include outpatient therapy, Intensive Outpatient Programs (IOPs), Partial Hospitalization Programs (PHPs), medication-assisted treatment (MAT), psychiatry, virtual behavioral health care, relapse prevention, and treatment for co-occurring mental health disorders. A major advantage is network access: Meritain says over 90% of its plan sponsors choose the Aetna Choice® POS II network, which includes 1.6 million providers and more than 350,000 behavioral health providers nationwide.
Outpatient care is often easier to access than residential rehab because it does not require 24/7 supervision, but higher-intensity outpatient programs like PHP and IOP may still require precertification or medical necessity review depending on the plan. Meritain’s precertification resources specifically note review requirements for mental health/substance use disorder care and residential treatment, and provider feedback online commonly says the biggest issue with Meritain is not whether outpatient care is covered, but how much the specific employer plan pays and whether authorization is needed. The best step is to have the outpatient rehab provider verify benefits, confirm Aetna network status, check copays/deductibles, and ask whether PHP, IOP, MAT, or virtual therapy require approval before treatment starts.
Additional Information about Meritain
One of the most important things to know about Meritain Health is that your employer, not Meritain itself, often has major control over how detox and rehab benefits are structured, because Meritain primarily administers self-funded employer health plans. This means two people with “Meritain” insurance can have dramatically different coverage for detox, residential rehab, PHP, IOP, out-of-network treatment, deductibles, and prior authorization requirements depending on where they work. Many people online mistakenly assume Meritain works like a standard national insurance company, but providers frequently note that understanding the employer-specific plan design is one of the biggest keys to avoiding unexpected rehab costs. This is why experienced rehab admissions teams almost always perform a full benefit verification instead of relying only on the insurance card.
Another very valuable thing many people do not realize is that Meritain members often gain access to one of the largest behavioral health provider networks in the country through the Aetna Choice® POS II network, which Meritain says includes over 350,000 behavioral health providers nationwide. This can make a major difference when searching for detox centers, dual diagnosis programs, psychiatrists, or specialized rehab providers because broader networks often reduce wait times and improve access to in-network care. Meritain is also somewhat unique among TPAs because it is the only third-party administrator with direct access to certain Aetna network solutions. Providers and members online often describe this as one of Meritain’s biggest advantages for behavioral healthcare, especially for people who may need to transition between detox, residential rehab, outpatient treatment, psychiatry, and ongoing therapy across different states or provider systems.
Personalize your treatment plan
with a benefits specialist. Call us.
Safely Detox at Castillian
Find Alcohol Treatment

Legacy Healing Center Parsippany, NJ

Legacy Healing Center Cincinnati, OH


