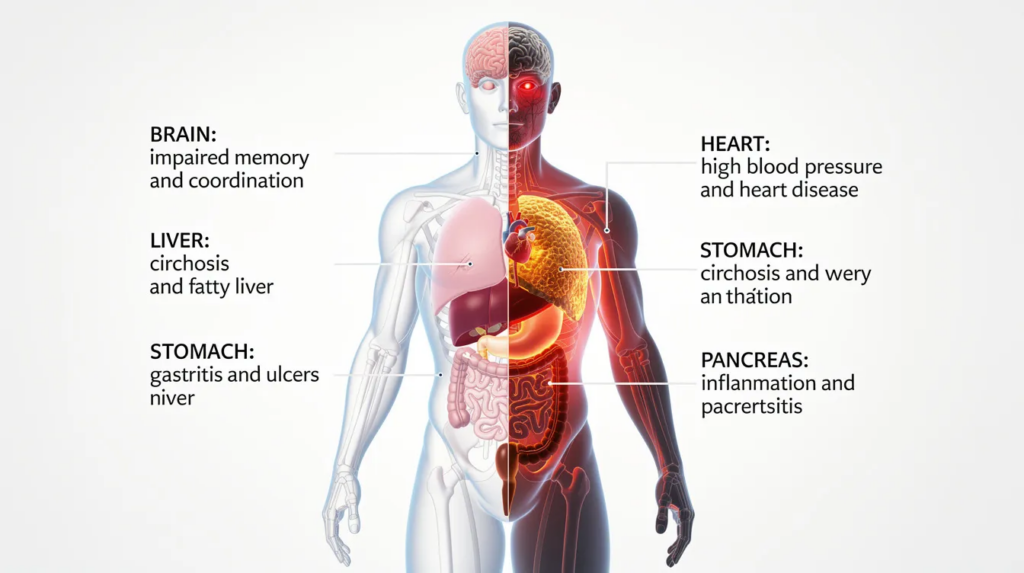
The Effects of Alcohol on the Brain and Body
-
 By:
Cody Perez
By:
Cody Perez
-
 Editor:
Phyllis Rodriguez, PMHNP-BC
Editor:
Phyllis Rodriguez, PMHNP-BC
-
 Clinical Reviewer:
Dr. Ash Bhatt, MD, MRO
Clinical Reviewer:
Dr. Ash Bhatt, MD, MRO
Understanding the effects of alcohol on the brain and body literally saved my life. As a certified addiction specialist with over 10 years in recovery, I’ve seen firsthand how drinking alcohol reshapes everything from your thinking to your heartbeat. In 2026, roughly 84% of adults report drinking alcohol at some point, and post-COVID data shows a 20-30% increase in high-risk drinking patterns that persists today.
Occasional, low-level alcohol consumption may not cause major harm for most healthy adults. But repeated heavy or binge drinking initiates cascading damage that many people don’t recognize until it’s advanced. This article has been medically reviewed with commentary by Dr. Ash Bhatt, a quintuple board-certified addiction physician at Legacy Healing Center. It will answer what alcohol is doing to your brain and body right now, then cover longer-term risks and treatment options.
How Alcohol Moves Through Your Body
When you take a drink, alcohol travels from your stomach and small intestine into your bloodstream, reaching your brain and other organs within minutes before the liver begins breaking it down.
- Alcohol is absorbed through the stomach lining (about 20%) and small intestine (80%), with effects on the brain within 5–10 minutes
- Peak blood alcohol concentration (BAC) occurs within 30–90 minutes depending on food intake, body weight, sex, and drinking speed
- The liver metabolizes roughly one standard drink (14 grams of pure alcohol—12 oz beer, 5 oz wine, or 1.5 oz spirits) per hour
- This rate varies based on genetics, liver health, age, and sex—women typically have higher BAC from the same amount of alcohol consumed
- Intoxication occurs when intake exceeds the body’s ability to metabolize, causing BAC to climb
- Alcohol is a small, water- and fat-soluble molecule that easily crosses the blood-brain barrier and placenta, posing risks during pregnancy
Your Brain on Alcohol: Short-Term Effects
Alcohol is a central nervous system depressant that interferes with the brain’s communication pathways by enhancing GABA (calming signals) and inhibiting glutamate (excitatory signals). This disruption affects brain cells throughout multiple regions.
- At low BAC (0.02–0.05): Prefrontal cortex inhibition causes you to feel relaxed, mildly euphoric, with lowered inhibitions and increased talkativeness
- At moderate BAC (0.06–0.15): Impaired judgment, slower reaction time, poor coordination, and increased risk of accidents and impulsive decisions
- At higher BAC (0.15+): The hippocampus cannot form new memories, causing blackouts—you may appear awake but form no memory of events
- Visible signs include slurred speech, blurred vision, balance problems, drowsiness, and slowed thinking
- Acute mental health effects: anxiety spikes, agitation, or aggression in some; alcohol temporarily numbs emotional pain but worsens mood swings afterward
I’ve experienced blackouts myself—waking up with no memory of entire conversations. That loss of control terrified me enough to seek help.
From “Buzzed” to Dangerous: Levels of Intoxication
Alcohol affects the nervous system in a dose-response pattern. These BAC ranges are general—individual responses vary significantly.
- Light (BAC 0.02–0.05): Mild warmth, slight mood lift, subtle decline in judgment
- Moderate (BAC 0.06–0.10): Clear impairment in driving ability, emotional swings, 4-10x higher crash risk
- Heavy (BAC 0.11–0.20): Major balance problems, slurred speech, blackouts, higher risk of fights, falls, unsafe sex
- Very high (BAC 0.21–0.30): Vomiting, confusion, inability to stand, risk of choking, hypothermia
- Life-threatening (BAC 0.31+): Alcohol poisoning, slow or irregular breathing, unresponsiveness, coma, potential death
Tolerance can mask visible signs—some heavy drinkers appear functional at dangerous BAC levels, but internal organ damage continues regardless.
Short-Term Risks: Accidents, Alcohol Poisoning, and Driving
Even one night of excessive drinking can have life-changing consequences. Alcohol contributes to approximately 30% of U.S. traffic fatalities—about 10,000 deaths annually at BAC ≥0.08.
- Falls account for 40% of alcohol-related ER visits; drownings are 50% alcohol-positive
- Violence, sexual assault, and unsafe sex risk increases dramatically with excessive alcohol use
- Alcohol poisoning is a medical emergency—signs include persistent vomiting, slow breathing (<8 breaths/min), blue skin, low body temperature
- First aid: Call 911 immediately, place person on their side, monitor airway—never “let them sleep it off”
- Mixing alcohol with opioids or benzodiazepines quadruples respiratory arrest risk
What Counts as “Too Much”? Binge Drinking and Alcohol Misuse
A standard drink in the U.S. is 12 oz beer (~5%), 5 oz wine (~12%), or 1.5 oz spirits (~40%). Many people underestimate their alcohol intake because typical pours exceed these amounts.
- Moderate drinking: Up to one drink per day for women, two for men—though no level is universally safe
- Binge drinking: Four or more drinks in about 2 hours for women, five or more drinks for men, bringing BAC to ~0.08
- Heavy drinking: 8+ drinks weekly for women, 15+ for men
- Age, sex, medications, liver health, and genetics all influence when too much alcohol becomes dangerous
- For those with liver disease, addiction history, heart conditions, or pregnancy—abstinence is safest
- Needing more alcohol to feel the same effect signals developing alcohol dependence
Long-Term Effects on the Brain and Mental Health
Repeated heavy drinking changes the brain’s chemistry, making alcohol feel necessary for normal function. This creates increased risk of lasting mental health problems.
- Chronic use disrupts GABA and glutamate, causing tolerance and withdrawal symptoms when not drinking
- Cognitive impacts: memory loss, attention difficulties, impaired problem-solving—sometimes persisting 1-2 years into sobriety
- Depression, anxiety, and suicidality risk increases 2-3x with alcohol misuse
- Wernicke-Korsakoff syndrome—a thiamine deficiency causing confusion, poor coordination, and severe memory problems—affects 10-30% of dependent drinkers
- Some brain damage reverses with sustained sobriety; severe cases can lead to permanent deficits
I experienced “brain fog” for months in early recovery. For many, mental clarity significantly improves with treatment—my thinking is sharper now than when I was drinking.
Long-Term Effects on Major Organs and Systems
Alcohol doesn’t only affect the brain. Over years, it quietly damages almost every organ, creating long term health risks.
- Liver: Progression from fatty liver → hepatitis → cirrhosis → liver failure and liver cancer (5x increased risk)
- Cardiovascular system: High blood pressure, heart disease, alcoholic cardiomyopathy (weakened heart muscle), heart attack, stroke
- GI/Pancreas: Gastritis, pancreatitis (potentially fatal), ulcers, malabsorption of essential nutrients
- Immune system: 3x higher risk of pneumonia; slower healing
- Bones/Muscles: Osteoporosis (25% bone loss), muscle wasting
- Cancer: Increased risk of mouth, throat, esophagus, colon, and breast cancer—even moderate alcohol use raises breast cancer risk 1.4x
Alcohol, Sleep, Hormones, Weight, and Immunity
Alcohol’s hidden effects show up daily as poor sleep, weight gain, and hormonal shifts that impact quality of life.
- Alcohol interferes with deep and REM sleep, causing night wakings and unrefreshing rest
- Hormones affected: cortisol (stress), testosterone (30-50% drop in chronic users), estrogen fluctuations
- At 7 calories per gram, alcoholic beverages contribute to weight gain and abdominal fat
- Immune function weakens with regular heavy drinking, increasing susceptibility to infections
- Chronic use worsens diabetes and metabolic conditions
Alcohol Withdrawal, Kindling, and Why Detox Can Be Dangerous Alone
In dependent drinkers, the brain adapts to constant alcohol, so suddenly stopping can trigger dangerous withdrawal symptoms. Never attempt detox alone if you have a history of heavy drinking.
- Early symptoms (6-24 hours): Tremors, anxiety, sweating, nausea, elevated heart rate, blood pressure spikes
- Severe symptoms: Hallucinations, seizures, delirium tremens (DTs) with fever and confusion—potentially life-threatening if left untreated
- “Kindling” effect: Each withdrawal cycle becomes more severe, doubling seizure risk
- Medically supervised detox uses medications to safely manage withdrawal and protect the heart and brain
Checking Your Drinking: Self-Assessment and Red Flags
Taking an honest look at your alcohol use is a sign of strength, not failure.
- Red flags: Needing alcohol to relax, drinking more than planned, hiding use, blackouts, relationship problems
- Validated screening tools like AUDIT or CAGE can help identify alcohol misuse
- Consequences—DUIs, missed work, worsening anxiety—often appear before physical illness
- If you cannot cut back despite wanting to, professional help is needed
When Alcohol Use Becomes Addiction (Alcohol Use Disorder)
Alcohol use disorder is a chronic medical condition—not a moral failing. It involves impaired control over drinking despite negative health consequences.
- Key features: Craving, loss of control, continued drinking despite harm, tolerance, withdrawal
- AUD exists on a spectrum from mild to severe AUD, and early intervention prevents many complications
- Trauma, genetics, and co-occurring conditions like PTSD commonly contribute
Recognizing my own AUD diagnosis was painful. But it became my turning point—and yours can be too.
Treatment Options: From Detox to Long-Term Recovery
Treating alcohol addiction involves stages: medical stabilization, intensive therapy, skill-building, and long-term support.
- Medically supervised detox: Safe withdrawal management over several days
- Residential/inpatient: 24/7 care with individual and group therapy
- Outpatient: PHP, IOP, or standard outpatient for those living at home
- Dual diagnosis: Treats co-occurring mental health conditions together
- Evidence-based approaches: CBT, motivational interviewing, medication-assisted treatment (naltrexone, acamprosate)
How Legacy Healing Center Approaches Alcohol Addiction
Legacy Healing Center is a luxury, accredited addiction and mental health treatment provider serving clients nationwide with comprehensive alcohol addiction care.
- Services: Medically supervised detox, residential rehab, PHP/IOP programs, aftercare, and sober living
- Led by Dr. Ash Bhatt, quintuple board-certified in addiction medicine
- Amenities: Private rooms, spa environment, gourmet meals, fitness programs, executive privacy
- Specialized programming: Dual diagnosis care, trauma-informed therapy, codependency treatment
- Same-day admissions available, insurance verification support, discreet travel concierge
Taking the Next Step: Getting Help for Alcohol Use
I know the fear, denial, and shame that keeps people drinking. Seeking help isn’t weakness—it’s the bravest thing you’ll ever do.
If you recognized yourself in any of these symptoms, reach out to Legacy Healing Center or a qualified addiction professional today. Many of alcohol’s effects on the brain and body can improve with sustained sobriety and good medical care.
Long-term recovery is possible. No one has to face this alone.









